If you suffer from severe, shooting pain that radiates from your lower back down through your hips and legs, you may have sciatica. This agonizing condition can make daily activities difficult and severely impact your quality of life. But where does this radiating leg pain come from? Surprisingly, arthritis is one of the top causes of sciatica.
Keep reading to understand the connection between sciatica and arthritis and what you can do to find relief. With the right information and treatment plan, you can get back to living your life unhindered by chronic back and leg pain.
What is Sciatica and What Causes It?
Sciatica refers to pain, numbness, or weakness that travels down the sciatic nerve, which runs from your lower back through your hips and butt and down each leg. While many equate sciatica with general back pain, true sciatica follows the specific path of the sciatic nerve.
Sciatica occurs when something compresses or irritates the sciatic nerve roots. Common causes include:
- Herniated (slipped) discs in the spine
- Spinal stenosis (narrowing of the spinal canal)
- Spondylolisthesis (slippage of one vertebra over another)
- Piriformis syndrome
- Spinal tumors or cysts
- Injury or trauma
One of the top causes of sciatica is arthritis in the spine. Let’s explore the connection between these painful conditions.
Can Arthritis Lead to Sciatica?
Arthritis, especially osteoarthritis, causes progressive damage to the joints, including the small facet joints in the spine. As these spinal joints break down, the vertebrae can shift and rub together. This puts pressure on the nerve roots, including those that form the sciatic nerve.
Osteoarthritis in the lower spine is a frequent cause of sciatica. The degenerating facet joints allow vertebrae to move out of place, which can directly compress or irritate the sciatic nerve. Damaged cartilage and bone spurs called osteophytes can also pinch nearby nerves.
Other types of spinal arthritis like rheumatoid arthritis and ankylosing spondylitis can cause inflammation in the vertebrae and discs. This leads to structural damage and narrowing of the areas where nerves exit the spine.
Ultimately, arthritis damages the spine and alters its normal structure. This can reduce space for nerves, leading to sciatica’s shooting pains.
How Does Arthritis Affect the Sciatic Nerve?
The effects of spinal arthritis eventually impact the bundle of nerves that make up the sciatic nerve. Arthritis affects this nerve in a few key ways:
| Cause | Description |
| Osteophyte formation | Bony spurs from osteoarthritis can directly pinch or rub on the sciatic nerve. |
| Inflammation | Swelling in the spine compresses the nerves and their roots. |
| Space loss | Narrowing between vertebrae leaves less room for the sciatic nerve to exit. |
| Nerve compression | Shifting vertebrae due to cartilage loss press on the nerve. |
| Referred pain | Arthritis around the sciatic nerve path sends pain signals down the leg. |
As arthritis damages the spine, the effects cascade outward to the web of nerves surrounding the spinal cord. This inevitably puts pressure on the sciatic nerve, producing pain.
How Does Arthritis in the Spine Lead to Sciatica?
Arthritis in the spine leads to sciatica through the gradual breakdown of the vertebrae and discs. This process include:
- Arthritis eats away spinal cartilage meant to cushion vertebrae. This causes bones to rub together.
- Loss of cartilage leads to formation of bony spurs called osteophytes. These spurs protrude into the spinal canal.
- Inflammation from spinal arthritis can also contribute to disc degeneration and nerve compression.
- As spinal arthritis advances, the vertebrae shift position, placing pressure on nerves. This directly irritates nerves like the sciatic nerve.
- All these factors – bone spurs, inflammation, and vertebral misalignment – pinch the sciatic nerve roots exiting the spine. This causes shooting leg pains.
Consequently, spinal arthritis and its effects on vertebral alignment are a prime cause of sciatica and its debilitating symptoms.
Treating Spinal Arthritis Causing Sciatica
If arthritis in your back or hips is causing sciatic pain, effectively managing the arthritis is critical to finding relief. Traditional sciatica treatments often fail because they don’t resolve the underlying arthritis.
Key approaches include:
1. Anti-inflammatory medications
Anti-inflammatory medications, specifically non-steroidal anti-inflammatory drugs (NSAIDs), can be used to reduce the inflammation and pain caused by arthritis. This category includes common OTC medications like ibuprofen, as well as prescription drugs.
2. Disease-modifying anti-rheumatic drugs (DMARDs)
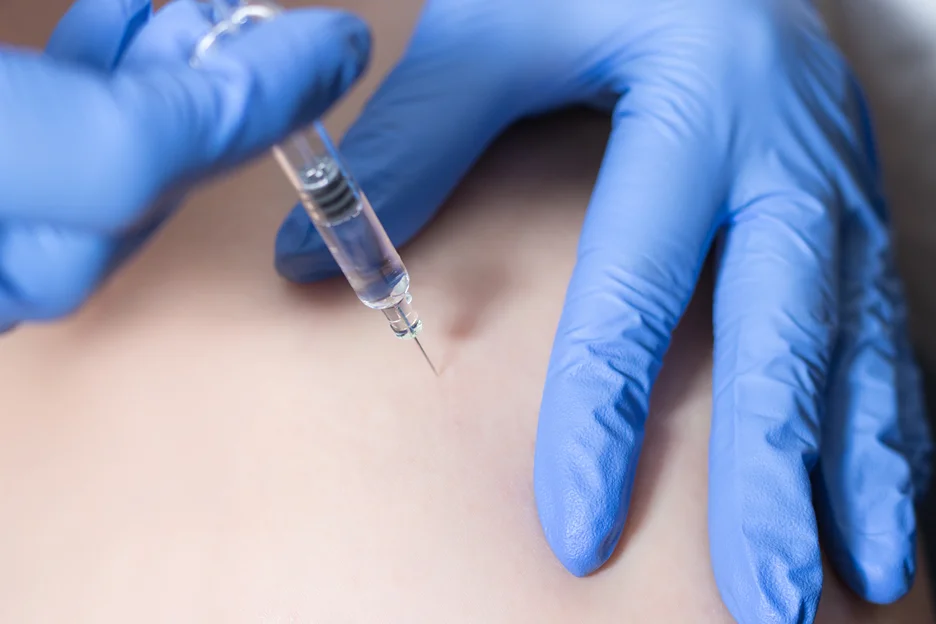
3. Epidural steroid injections
DMARDs work by slowing down the progression of arthritis, rather than simply managing symptoms. They do this by modifying the immune system, which can help reduce inflammation in the joints.
Epidural steroid injections involve delivering a steroid medication directly into the epidural space, which is the area around the inflamed spinal nerves. This can help to reduce inflammation and provide localized pain relief. This is usually a short-term solution and can be used in conjunction with other treatments.
4. Physical Therapy
Physical therapy can be an important part of managing sciatic pain caused by spinal arthritis. This can involve a range of activities including stretching and strengthening exercises, applying heat or ice, and learning proper movement patterns to avoid aggravating the condition. The goal of physical therapy is not only to manage symptoms but also to improve the patient’s ability to perform daily activities.
5. Spinal decompression surgery
In severe cases of spinal arthritis causing sciatica, spinal decompression surgery may be an option. The goal of this type of surgery, including procedures like a laminectomy, is to relieve pressure on the nerves in the spine. This is usually considered a last resort when more conservative treatments have failed.
6. Lifestyle modifications
Making lifestyle changes can also help to manage sciatic pain caused by spinal arthritis. This could include losing weight to reduce stress on the joints, using proper posture and body mechanics, and avoiding activities that aggravate symptoms. Other lifestyle changes might include quitting smoking, eating a healthy diet, and getting regular exercise.
7. Alternative therapies
Finally, some patients might find relief from alternative therapies. This could include treatments like:
- Acupuncture which involves inserting thin needles into specific points on the body
- Massage which can help to relieve muscle tension
- Chiropractic adjustment which involves manipulating the spine to improve alignment and relieve pain.
It’s important to note that while these treatments can be beneficial, they should be used in conjunction with traditional medical treatments, rather than as a substitute.
The Takeaway: Arthritis is a Common Cause of Sciatica

While sciatica has numerous potential causes, arthritis in the spine and hips is one of the top contributors to this radiating leg pain. Seeking an accurate diagnosis is the first step to finding real relief.
If imaging reveals spinal arthritis compressing the sciatic nerve roots, treating the arthritis is key to calming inflammation and taking pressure off the irritated nerves.
Your doctor can help formulate a treatment plan that fits your specific case of sciatica and spinal arthritis. This may include medications to reduce inflammation along with physical therapy to improve joint flexibility and spinal alignment.
You deserve to live free from the misery of sciatica. By understanding the connection between your spinal arthritis and nerve irritation, you can take steps to properly care for your back and nerves. Support structures like Kaly make it simple to connect to top specialists and access personalized treatment programs right from your home.
Sign up for Kaly to get matched with arthritis and sciatica resources and start feeling better soon.
Frequently Asked Questions
Is an Arthritic Hip a Common Cause of Sciatica?
An arthritic hip joint is another frequent source of sciatic pain. Like other joints, osteoarthritis in the hip causes cartilage breakdown. As the hip joint space narrows, the arthritic ball and socket rub together. This causes bone spurs around the hip joint.
The inflamed arthritic hip area can put pressure on the nearby sciatic nerve. Bone spurs can also impinge the nerve. This hip-driven irritation produces sciatica-like symptoms down the leg.
So while the primary cause is hip arthritis versus spine arthritis, the end result is similar – the sciatic nerve gets pinched, leading to radiating leg pains.
Can Rheumatoid Arthritis Cause Sciatica?
Rheumatoid arthritis is another potential cause of sciatica. RA targets the synovial membranes lining joints, but it can also affect tissues throughout the body. When RA impacts the spine, it attacks the vertebrae, discs and ligaments.
The inflamed tissues swell and expand into the spinal canal. RA also progressively damages spinal bones and discs. All this structural damage and inflammation in the spine from RA can irritate, compress, and damage the sciatic nerve roots. As with osteoarthritis, rheumatoid arthritis in the spine frequently contributes to sciatica.
Studies estimate the prevalence of peripheral neuropathy in rheumatoid arthritis patients to be around 50%, with carpal tunnel syndrome and polyneuropathy being most common. Sciatica has been reported in 13-30% of rheumatoid arthritis patients, as inflammation can irritate the sciatic nerve.
Can Arthritis in the Knee Trigger Sciatica?
Knee arthritis won’t directly cause classic sciatica, but it can contribute to radiating leg pains. The sciatic nerve runs down the back of the thigh and calf, so knee arthritis won’t impact the nerve itself.
However, arthritic knees can cause referred pain signals that travel down the leg in a sciatica-like pattern. Knee arthritis may also lead to impaired mobility, resulting in more back strain and nerve compression.
So while knee arthritis won’t compress the sciatic nerve, it can still produce symptoms resembling sciatic pain that spreads from the lower back down the leg.
Is it Common to Have Both Arthritis and Sciatica?
Having both arthritis and sciatica is certainly possible, but not overly common. These conditions frequently occur on their own.
However, spinal arthritis is one of the top preventable causes of sciatica. When arthritis damages spinal bones and tissues, it affects the delicate nerve roots traveling through the vertebral column.
Likewise, sciatica can lead to immobility and added spinal stress. This may accelerate arthritis progression. The two conditions influence each other, so having both simultaneously does occur. But other factors like disc herniation are more often to blame for sciatica.
Getting an accurate diagnosis is key to finding the right treatments to resolve chronic back and leg pain. Seeing a specialist can help identify the specific cause.
Can Arthritis Aggravate Existing Sciatica?
If you already have sciatica, worsening arthritis can definitely exacerbate your symptoms. Sciatica makes the spinal nerves more sensitive to any source of compression or inflammation.
Advancing arthritis in the spine squeezes nerves already inflamed from sciatica. Small amounts of bone growth or swelling from arthritis can flare up severe sciatic pain.
Arthritis also accelerates degenerative processes like disc deterioration, reducing available space for the sciatic nerve. Existing sciatica coupled with progressive arthritis typically amplifies radiating leg pains.
